The federal data behind your worst sleep problem
BLS data on shift and flexible schedules confirms what millions of nurses, warehouse sorters, long-haul truckers, emergency dispatchers, and manufacturing line workers already feel at 3 a.m.: a significant portion of the U.S. workforce operates on schedules that are biologically incompatible with healthy sleep. This is not a lifestyle complaint. It is an occupational hazard with a federal paper trail.
NIOSH research on shift work and long work hours classifies sleep deprivation arising from non-standard schedules as a measurable workplace hazard — one with documented downstream injury rates, accident risk, and long-term health consequences. Meanwhile, CDC sleep statistics show that roughly 1 in 3 U.S. adults already fails to get the recommended 7 or more hours per night across all occupations. For shift workers, who are fighting their own biology to sleep at the wrong time, that number is meaningfully worse.
The downstream costs are not theoretical. BLS Workers' Compensation data captures elevated injury rates in transportation and healthcare — two of the largest shift-work sectors — where fatigue-linked errors translate directly into on-the-clock incidents. The FMCSA hours-of-service regulations exist precisely because federal crash data established a direct, quantifiable link between driver fatigue and crash risk. Federal regulators do not cap commercial driver hours because of general wellness concerns. They do it because tired shift workers kill people, including themselves.
NIH NHLBI estimates that 50 to 70 million U.S. adults have a chronic sleep or wakefulness disorder — a number large enough that addressing it is a genuine public health priority, not a niche wellness market. The NIOSH Total Worker Health program formally frames sleep as an occupational health variable, not a personal-life issue that workers manage on their own time. That framing matters: it means interventions — behavioral, environmental, clinical, and technological — all belong in the same conversation.
Why shift work breaks sleep at the biological level
The human circadian system is not a metaphor. It is a real, hormone-driven biological clock anchored to light exposure. The suprachiasmatic nucleus in the hypothalamus receives photic input from the retina and uses it to synchronize melatonin secretion, cortisol rhythm, core body temperature cycling, and dozens of downstream physiological processes. The system evolved over hundreds of thousands of years in which light reliably predicted daytime and dark reliably predicted nighttime. Shift work breaks that contract completely.
When a night-shift nurse finishes a 12-hour rotation at 7 a.m. and drives home into full sunlight, her retinal photoreceptors are receiving the exact signal that tells her brain it is time to be awake and alert. Cortisol is still elevated from the morning surge. Core body temperature is rising. Melatonin secretion has already been suppressed by ambient light. She is trying to sleep in a body that is hormonally and neurologically configured to do the opposite.
The result is delayed sleep onset — the time between lying down and actually falling asleep stretches from the normal 10-to-20 minute range into 45 minutes, an hour, or longer. When she finally does sleep, the architecture is disrupted: less slow-wave deep sleep, fewer complete REM cycles, more fragmented wakefulness. Total sleep time is compressed. Sleep quality declines. And crucially, this is not a one-night problem. Rotating schedules, irregular shift assignments, and chronic misalignment accumulate as what researchers call social jetlag — a persistent, chronic desynchronization between the body's internal clock and the external schedule imposed by work.
For workers on permanent night shifts, the picture is marginally better — the body does eventually shift its circadian phase somewhat — but full adaptation rarely occurs because most workers revert to daytime schedules on days off. The circadian clock cannot adapt to a target that keeps moving.
NIOSH's occupational health framework documents the consequences beyond just feeling tired: elevated rates of metabolic syndrome, cardiovascular disease, gastrointestinal disorders, and psychiatric conditions all track with long-term shift work exposure. The injury risk is immediate; the health consequences accumulate over years.
The cheapest intervention is the one that requires no purchase
Before any discussion of technology, the evidence base is unambiguous: behavioral and environmental interventions have the strongest effect sizes for shift-worker sleep problems, and most of them are free. Federal guidance from CDC and NIH is specific and actionable.
CDC sleep hygiene guidance identifies the bedroom environment as the single most modifiable variable for sleep quality: keep the room between 65 and 68 degrees Fahrenheit, make it blackout dark, eliminate screens for at least one hour before your intended sleep time, and maintain a consistent wake time. These are not vague suggestions. They are evidence-based environmental parameters that directly address the biological mechanisms disrupting shift-worker sleep — particularly light exposure and thermal regulation, both of which are inputs to the circadian clock.
NIOSH guidance specifically for shift workers goes further: blackout curtains, eye masks, and aggressive noise reduction during daytime sleep periods are categorized as primary interventions, not optional comfort upgrades. Light exposure during off-shift sleep is the dominant driver of chronic shift-worker sleep deficit. Addressing it with blackout curtains costs approximately $25 to $40 per window. No wearable or smart device produces an equivalent effect per dollar spent.
NIH NHLBI sleep guidance emphasizes that consistent timing — same bedtime, same wake time, seven days a week — has stronger effects on sleep quality than chasing extra hours on weekends. For shift workers on rotating schedules, perfect consistency is impossible. But anchoring the sleep window as tightly as possible, even when the absolute clock time shifts, provides partial circadian stabilization. Technology that enforces that consistency — a dawn-simulating alarm that wakes you at the same biological phase each cycle — earns its place. Technology that merely measures your poor sleep and tells you it was poor does not.
CDC adult physical activity guidelines recommend 150 minutes of moderate-intensity activity per week. Multiple cohort studies associate meeting that threshold with improved sleep latency and sleep quality. For shift workers whose schedules make gym access erratic, the practical implication is that movement during any available waking window is a sleep input, not just a cardiovascular one. Walking, cycling, or resistance training during the hours before your intended sleep window should be timed to avoid the alerting effect of exercise too close to sleep, but the weekly accumulation matters regardless of when individual sessions occur.
Finally, before spending a dollar on sleep technology, NHLBI sleep apnea screening criteria make clear that loud snoring, witnessed apneic episodes (pauses in breathing), unrefreshing sleep, morning headaches, and excessive daytime sleepiness are clinical symptoms that warrant a formal sleep study. Shift workers experience daytime sleepiness as a baseline — which can mask apnea symptoms for years. CDC adult obesity data shows approximately 40% adult obesity prevalence, and obesity is the leading modifiable risk factor for obstructive sleep apnea. A smart ring or sleep mask does not diagnose or treat sleep apnea. A polysomnogram and a CPAP machine do.
For readers who have addressed the bedroom environment, established what consistency is possible given their schedule, ruled out clinical sleep disorders, and still find sleep onset and quality falling short: this is the space where sleep technology has a legitimate, evidence-adjacent role. The products below were selected specifically for shift workers — not general consumers — based on the mechanisms that matter for this population: thermoregulation, circadian light signaling, and objective sleep-phase tracking.
When to see a clinician — and what the red flags look like
Sleep technology is not a substitute for clinical evaluation, and for a meaningful subset of shift workers, the problem they are trying to solve with gadgets is actually a diagnosable disorder that requires medical treatment.
NHLBI sleep apnea guidance lists the red flags clearly: snoring loud enough to disturb a bed partner, observed pauses in breathing during sleep, waking with a choking or gasping sensation, persistent morning headaches, and daytime sleepiness that impairs function despite adequate time in bed. These symptoms, especially in combination, indicate a high pretest probability of obstructive sleep apnea. For shift workers, the overlap with normal shift-work fatigue is significant — which is exactly why systematic screening matters before attributing all symptoms to schedule disruption. Untreated sleep apnea raises cardiovascular risk substantially and is not addressed by any consumer sleep device.
NIH NHLBI estimates that the 50-to-70 million Americans with chronic sleep or wakefulness disorders include large numbers of undiagnosed cases. Shift Work Sleep Disorder (SWSD) is itself a clinical diagnosis in the International Classification of Sleep Disorders — characterized by insomnia and/or excessive sleepiness that is temporally linked to a recurring work schedule. If symptoms persist despite optimized sleep hygiene and schedule management, an occupational medicine physician or sleep specialist is the appropriate next step, not a more expensive wearable. NIOSH Total Worker Health guidance explicitly supports employer-facilitated access to sleep health screening for shift workers — meaning your employer may have an obligation to help fund the evaluation.
Where technology earns its place for shift workers
With free interventions implemented and clinical conditions ruled out or managed, a targeted set of sleep technologies addresses the specific biological mechanisms that shift work disrupts. The products worth considering for this population fall into three functional categories: active thermoregulation, circadian light signaling, and physiological recovery tracking.
Active thermoregulation: Eight Sleep Pod 4 Cover
Core body temperature drop is one of the primary physiological triggers for sleep onset. In a well-functioning circadian system, core temperature begins falling approximately two hours before your habitual bedtime. In a shift worker who just drove home into morning sunlight, that temperature signal is suppressed or phase-shifted. You cannot force melatonin secretion, but you can actively lower your sleep surface temperature to replicate the environmental cue the body is missing.
The Eight Sleep Pod 4 Cover is the most clinically coherent piece of consumer sleep technology for this application. It uses active water circulation to control mattress surface temperature with precision — cooling the bed to accelerate sleep onset, warming it in the early morning to ease the wake transition — and it does this automatically based on individual sleep-stage data. For a nurse finishing a night shift at 7 a.m. and needing to sleep by 8:30 a.m. in a warming house, a cooling sleep surface is not a luxury feature. It is a direct intervention on one of the two primary circadian inputs (light and temperature) that make daytime sleep hard. At $2,049 to $5,049 depending on configuration, this is not a casual purchase — but among all consumer sleep devices, it addresses the most specific biological mechanism relevant to shift-worker sleep onset failure.
Recovery tracking: Whoop 4.0
Shift workers do not always know which part of their schedule is doing the most damage. Is it the 4 a.m.-to-noon rotation, or the 2-to-10 p.m. swing? Is the weekend schedule reversal costing more recovery than the mid-week overnight? The Whoop 4.0 was designed as a continuous physiological monitoring system — tracking heart rate variability, respiratory rate, sleep stages, and recovery strain — and it surfaces that data in a way that lets workers identify which schedule patterns are extracting the highest physiological cost.
Whoop's sleep-coaching feature accounts for sleep debt accumulated across days, not just the previous night — a meaningful design choice for shift workers who build chronic debt over rotations. The subscription model ($239 for the band plus an ongoing membership fee) is a real consideration, but for workers who need to make a case to a manager for schedule modification, or who are tracking recovery after a health event, objective HRV and sleep-stage data have practical value beyond personal curiosity.
Circadian light signaling: Hatch Restore 3
Dawn simulation is one of the few consumer sleep interventions with a coherent biological mechanism and a genuine body of supporting research. Gradual light exposure in the 20-to-30 minutes before a target wake time partially substitutes for natural dawn, triggering cortisol awakening response and advancing circadian phase. For shift workers whose "dawn" occurs at 2 p.m. or whose schedule forces a wake time after six hours of daytime sleep, this matters.
The Hatch Restore 3 Sunrise Alarm Clock provides programmable dawn simulation with customizable light temperature and intensity, paired with sound environments for both sleep onset and wake. At $169.99, it is the most accessible product in this set and addresses the circadian light-signaling mechanism directly. For shift workers who have already implemented blackout dark for sleep but need a physiologically appropriate light signal to initiate waking — without the jarring cortisol spike of a standard alarm — the Hatch Restore 3 is the highest-value starting point.
Sleep Tech Built for the Specific Problems Shift Workers Face
These three products were selected for shift workers specifically — each addresses a distinct biological mechanism that non-standard work schedules disrupt: core body thermoregulation, circadian light signaling, and physiological recovery tracking.
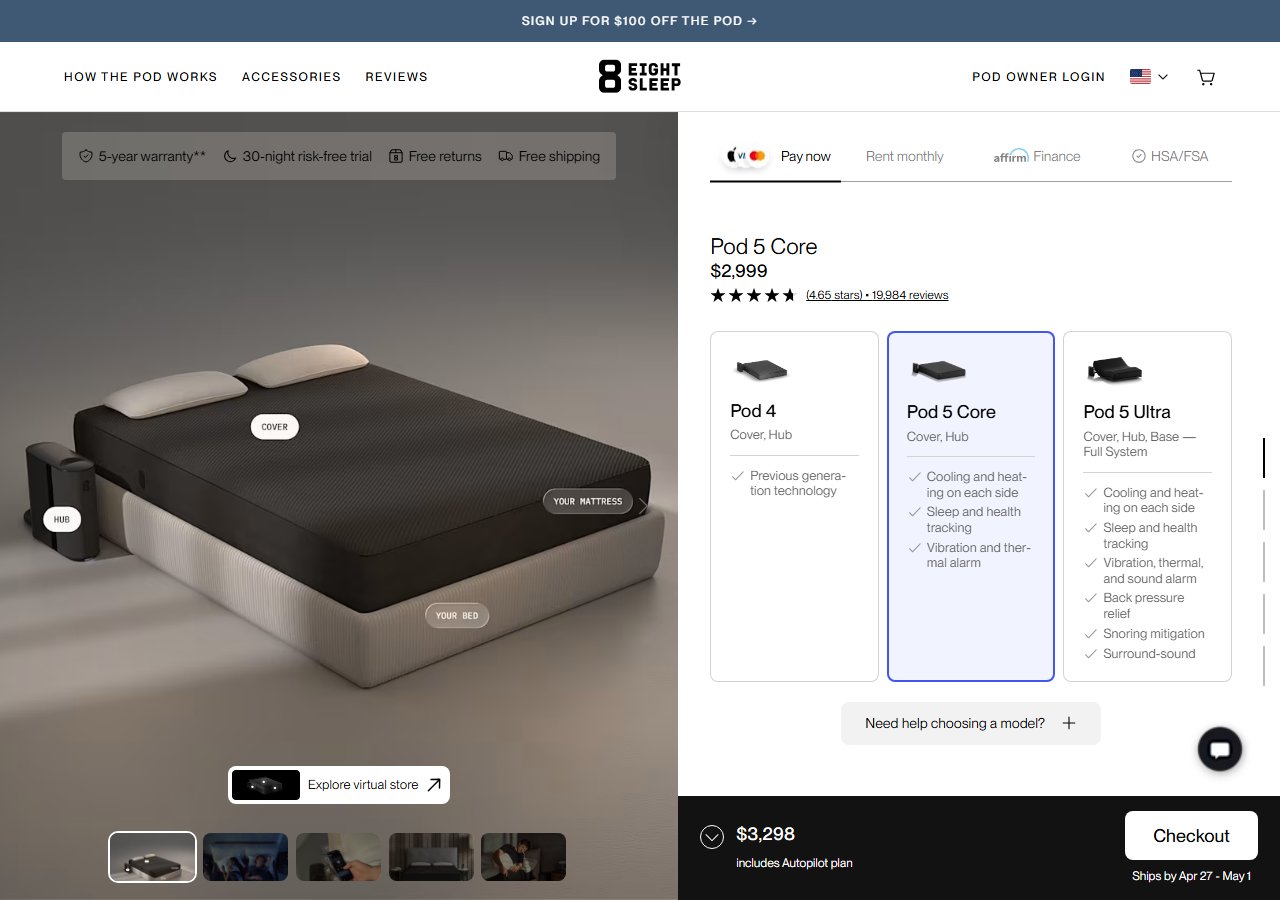
Eight Sleep Pod 4 Cover
$2,049-$5,049
See Price at Eight Sleep →
Whoop 4.0
$239 + subscription
See Price at Whoop →
Hatch Restore 3 Sunrise Alarm Clock, Sound Machine, Smart Light (Putty) - Whi...
$169.99
Check Price on Amazon →The hierarchy that actually works
Federal data tells a consistent story: shift work creates occupational sleep disruption at a population scale, the consequences are measurable in injury rates and accident data, and the interventions that work best are behavioral and environmental before they are technological. NIOSH Total Worker Health guidance frames this as an employer responsibility as well as an individual one — workers should not have to purchase their way out of a hazard that scheduling creates.
The practical hierarchy for shift workers is:
- Fix the bedroom environment first. CDC sleep hygiene guidance — cool, dark, screen-free — addresses the same circadian inputs that every expensive device is also trying to address, at near-zero cost.
- Anchor your sleep timing as tightly as your schedule allows. NHLBI's guidance on consistent timing has stronger evidence than total hours for sleep quality outcomes.
- Screen for clinical disorders before buying gear. Loud snoring, daytime sleepiness, and unrefreshing sleep in a worker with any obesity-related risk factors warrant a sleep study, not a wearable.
- Move your body during available waking hours. CDC physical activity guidelines associate 150 minutes per week of moderate activity with improved sleep latency. Movement is sleep technology.
- Add targeted devices for the specific mechanisms still failing. If sleep onset remains difficult after environmental optimization, active thermoregulation via the Eight Sleep Pod 4 Cover addresses that mechanism directly. If circadian wake signaling is the problem, the Hatch Restore 3 provides dawn simulation at accessible cost. If you need to understand which schedule patterns are costing you the most recovery, the Whoop 4.0 provides that physiological visibility.
None of these devices replaces what the free interventions do. All of them work best in an environment where the behavioral and environmental foundations are already in place. That is not a caveat — it is the mechanism. Sleep technology is an adjunct to sleep hygiene, not a replacement for it.